Directed Payments - A Lifeline for Rural Healthcare
Rural hospitals face a perfect storm of challenges: aging populations, higher rates of chronic disease, lower reimbursement rates, and thinner operating margins. The Medicaid Directed Payment Program has emerged as a critical tool to ensure these essential healthcare facilities remain viable while improving care quality. Nebraska's recent implementation offers valuable insights into how these programs can transform rural healthcare delivery.
Directed payments, established by the Centers for Medicare & Medicaid Services (CMS) in 2016, allow states to require Medicaid managed care organizations (MCOs) to pay providers according to specific rates or methods. According to MACPAC (Medicaid and CHIP Payment and Access Commission), these payment arrangements can be used to establish minimum fee schedules, require participation in value-based payment arrangements, or implement uniform payment rate increases. Unlike traditional supplemental payments, which aren't allowed in managed care, directed payments must be tied to utilization and delivery of services under the managed care contract, distributed equally to specified providers, and advance at least one goal in the state's managed care quality strategy.
Safeguarding Healthcare's Future - “Investment Lessons from Warren Buffett's 2024 Letter”
With Berkshire Hathaway reporting $47.4 billion in operating earnings for 2024, Warren Buffett's latest insights offer timely lessons for healthcare organizations aiming to strengthen their investment programs. Hospitals and health systems face unique challenges: they must balance strict regulatory requirements, credit rating considerations, and community care obligations while pursuing long-term financial stability.
One of Buffett's most pointed observations centers on the vulnerability of paper currency. "Paper money can see its value evaporate if fiscal folly prevails," he warns, noting that "in some countries, this reckless practice has become habitual." This caution is particularly relevant for hospitals, which typically hold substantial cash reserves to ensure smooth operations and manage major capital expenditures. Although liquidity is critical, a heightened awareness of inflation and currency risk calls for more sophisticated cash management strategies. Importantly, Buffett notes that "Fixed-coupon bonds provide no protection against runaway currency," suggesting the need for more dynamic approaches to preserving purchasing power.
The State of Rural Healthcare
The state of rural healthcare in America has reached a critical tipping point, with nearly half of rural hospitals operating in the red and 432 facilities vulnerable to closure. According to the Chartis report, these stark numbers represent more than just statistics – they reflect a growing crisis in healthcare access for over 46 million Americans living in rural communities.
Since 2010, 182 rural hospitals have either closed their doors completely or converted to models that no longer provide inpatient care. This represents approximately 10% of the nation's rural hospitals, creating what healthcare experts call "care deserts" across vast stretches of rural America. The impact is particularly severe in states like Texas, which has lost 26 facilities, and Tennessee, which has seen 16 closures.
Market Overvaluation and the Case for Value-Based Hospital Investment: Lessons from the Buffett Indicator
Healthcare organizations face a critical juncture in their investment and operational strategies. The Buffett Indicator, a metric for assessing market valuations, tells a compelling story: with a current reading of 208%, the total U.S. stock market value towers at more than double the nation's GDP. This stark figure, sitting approximately 66.62% above the historical trend line, signals that the market is strongly overvalued and demands attention from hospital leadership.
For healthcare organizations, particularly hospitals that typically maintain substantial investment portfolios, this market environment presents both challenges and opportunities. Recent market events provide a stark illustration of this fragility. Consider the impact of Deepseek's emergence just last month, when this Chinese AI company's release of competitive large language models challenged a fundamental market assumption: the perceived invulnerability of U.S.-based AI companies. For years, American technology giants had justified their extraordinary valuations partly on the notion of an unassailable AI moat – a combination of data advantages, computational resources, and intellectual capital that investors believed would be nearly impossible for competitors to replicate.
When Deepseek demonstrated comparable capabilities at a fraction of the development cost, it exposed the fragility of these assumed competitive advantages. Major American tech companies, which had commanded premium valuations based on their perceived AI dominance, saw their market capitalizations decline significantly as investors were forced to reassess their assumptions about technological barriers to entry. This episode demonstrated not just how quickly market sentiment can shift, but how dangerous it can be to build investment theses on perceived competitive advantages that may prove more vulnerable than expected.
Quality, Patience, and Purpose - What Hospitals Can Learn from Charlie Munger
Charlie Munger’s life is a masterclass in disciplined thinking, patience, and the pursuit of quality. As Warren Buffett’s partner at Berkshire Hathaway, Munger’s influence shaped not only one of the most successful investment strategies in history but also a broader philosophy of decision-making that resonates far beyond finance. His approach offers lessons for individuals and organizations alike—particularly those navigating complex and mission-driven challenges.
Munger’s principles were forged early in life, rooted in values of fairness, self-control, and intellectual curiosity. Raised in a modest but loving home, he was instilled with the importance of education and the discipline to pursue meaningful goals. These lessons carried through his career, where he became known for his emphasis on making decisions based on enduring value rather than fleeting trends.
The $51 Million Opportunity - Minnesota Hospitals' Untapped Investment Potential (Part 2)
As a follow-up to Tuesday’s (Dec 10) post, we presented an opportunity many hospitals have available through a strategic approach to managing the balance sheet financial assets. Hospitals continually search for ways to strengthen their financial foundation. To recap, a recent analysis of 37 Minnesota hospitals has uncovered a significant opportunity many institutions overlook: again - through a more strategic utilization of their investment portfolios.
These 37 hospitals collectively manage nearly $1 billion ($933.5M) in investable assets, yet currently generate only $13.9 million in annual investment income—a return of just 1.49%. With current treasury rates between 4-5%, even a conservative treasury strategy could generate between $37.3 million and $46.7 million annually—an additional $23.4M to $32.8M over current returns. This represents an additional $632,000 to $886,000 per hospital, achievable through low-risk treasury management. To put this in perspective, even at the conservative 4% return level, the additional $23.4M in annual income could fund 195 new nursing positions across these institutions. Moving to a balanced portfolio approach targeting 7% returns would generate $65.3 million annually, providing an additional $51.4M system-wide or $1.4M per hospital through a thoughtfully diversified investment strategy.
The most overlooked opportunity for Rural Hospitals - One State’s example
Hospitals have traditionally focused on operational revenue for much of their ability to reinvest in the resources needed to care for a community—the day-to-day revenue (and income) from patient care, procedures, and reimbursements. But beneath these obvious revenue streams lies a potentially transformative opportunity that many healthcare institutions overlook: the strategic management of their investable assets.
A recent study of 37 Minnesota hospitals reveals a striking picture of this untapped potential. These institutions collectively manage nearly $1 billion in investable assets. Yet, their cautious investment approaches may leave significant value on the table—value that could be reinvested in patient care, staff development, and crucial infrastructure improvements.
Understanding America's National Debt Interest Costs
Picture this: For every tax dollar you send to Washington in 2024 (soon to be 2025), a growing portion isn't going to provide healthcare, build highways, support veterans, or fund education. Instead, it's being used to pay interest on our national debt. According to recent Congressional Budget Office projections, this year alone, the federal government will spend an astounding $892 billion just on interest payments. That's not paying down the debt itself – that's merely the cost of borrowing.
To grasp the magnitude of this financial burden, consider that we're now spending more on interest payments than on Medicaid, all federal programs for children, veterans' benefits, and critical income security programs combined. These interest payments, which essentially amount to the cost of past spending, are beginning to overshadow investments in our nation's future.
Value-Based Investing - The Strategic Alignment with Hospital Mission
In hospitals today, administrators and board members face a unique challenge: balancing the noble mission of healthcare delivery with the pragmatic needs of financial sustainability. This intersection of purpose and practicality finds a compelling solution in an investment philosophy that dates back to the Great Depression – value investing.
Benjamin Graham, often called the father of value investing, developed his investment principles during one of America's most challenging economic periods. His approach, first detailed in "Security Analysis" (1934), emphasized finding the true worth of investments beyond their market prices. This focus on intrinsic value mirrors how hospitals must evaluate both their clinical and financial decisions – with careful analysis, patient consideration, and a long-term perspective.
Howard Marks, a modern torchbearer of value investing principles, wrote in "The Most Important Thing" (2011) that "successful investing requires thoughtful attention to many separate aspects, all at the same time." This multifaceted approach resonates deeply with hospital operations, where success depends on simultaneously managing patient care, financial stability, and community health.
Part 5: Monitoring Performance and Adapting to Changing Market Conditions
Even with a well-defined financial strategy, ongoing monitoring, and adaptability are essential to ensure long-term success. Market conditions fluctuate, and healthcare needs evolve, necessitating a proactive approach to managing financial assets.
Regular performance reviews are essential to aligning with the hospital’s mission and goals. Monitoring helps ensure that investments continue to meet targeted returns and that assets are being optimally utilized to support operational and capital needs.
Part 4: Governance and Fiduciary Responsibility in Asset Management
Introduction As hospitals increasingly rely on financial assets to support their missions, strong governance and fiduciary oversight become crucial. Effective asset management requires more than sound investments; it also requires a commitment to transparency, accountability, and adherence to fiduciary best practices.
The Role of Fiduciary Responsibility For hospitals, fiduciary responsibility means managing assets with the highest ethical standards and ensuring that investments are made in the best interest of the organization and its community. Adhering to standards like the Uniform Prudent Management of Institutional Funds Act (UPMIFA) provides a legal and ethical framework for responsible financial management.
Part 3: Aligning Financial Strategy with Operating and Capital Needs
Introduction Balancing operational and capital needs is a critical challenge for hospitals. As costs rise and reimbursements fluctuate, hospitals are often forced to make difficult choices between day-to-day operating needs and long-term capital improvements. One solution to this dilemma is optimizing balance sheet assets to generate a reliable revenue source that supports both immediate and future needs.
Why Alignment Matters Hospitals must be able to cover both daily expenses and long-term investments, such as facility upgrades, technology, and staff development. By strategically investing the financial reserves, hospitals can create a dedicated source of revenue that helps balance these needs, reducing the dependency on inconsistent operating income alone.
Part 2: The Case for Value-Based, Fundamental Investing in Healthcare
Introduction For years, many hospitals have taken a conservative approach to financial management, prioritizing asset protection with low-yield investments. While safe, this approach no longer meets the demands of today’s healthcare environment. Hospitals need a strategy that balances stability with growth—a value-based, fundamental approach that aligns with their mission and financial needs.
What is Value-Based, Fundamental Investing? Value-based, fundamental investing is an approach focused on long-term growth by investing in quality assets that are undervalued in the market. Rather than seeking short-term gains, this strategy prioritizes stability and alignment with the hospital’s goals, such as supporting healthcare innovation, community health, and financial resilience.
Series Title: Strategic Balance Sheet Management: A Guide for Sustainable Hospital Growth
The financial landscape grows more challenging each year for hospitals, particularly those serving rural communities. Hospitals are increasingly pressured to do more with less with less - with declining reimbursement rates, rising operational costs, and a complex regulatory environment. Over the last two decades, over 180 hospitals closed nationwide—often leaving communities without access to essential healthcare services.
In response to these challenges, some healthcare leaders often overlook a valuable resource: balance sheet financial assets. When managed strategically, these assets can become a sustainable source of non-operating revenue, creating financial resilience and supporting reinvestment in patient care, staff, and critical infrastructure.
What’s Better? Maximizing Operating Income or Strategic Balance Sheet Management
Hospitals face mounting financial pressures: declining reimbursement rates, rising operating costs, and an ever-growing demand for high-quality, patient-centered care. This reality has made it increasingly challenging for hospitals to sustain their operations solely through traditional income sources. In response, many hospital leaders are asking a crucial question: “Is there a better way to support our mission than relying on operating income alone?”
This question opens the door to an alternative approach—strategic balance sheet management. By optimizing financial assets for long-term investment, hospitals can create an additional, sustainable source of non-operating income, allowing them to reinvest in resources, staff, and services that directly benefit their communities.
In this post, we’ll explore how each approach can impact a hospital's financial outlook over the long term. We’ll look at the potential for operating income alone versus a value-based investment strategy for balance sheet assets. Using hypothetical but realistic assumptions, we’ll outline which path yields the best financial support for the organization’s mission over the next 10 and 20 years.
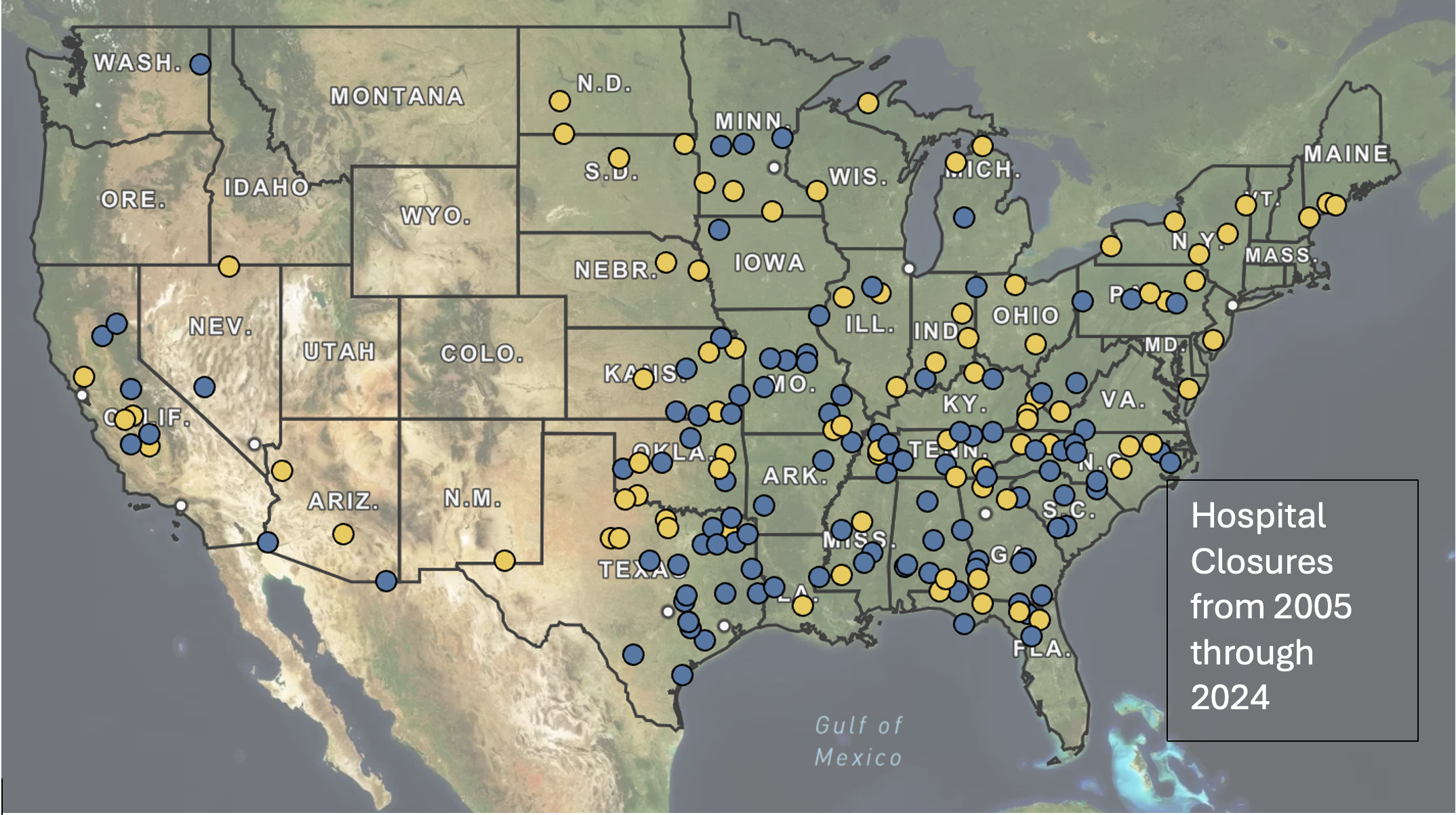
Looming Crisis of Rural Hospital Closures - A New Model Sheds Light on Financial Distress
Rural hospitals are more than healthcare providers—they are pillars of their communities. They serve as key employers (generally one of the top three employers within the community), lifelines during emergencies, and providers of essential medical care. However, the ongoing wave of rural hospital closures threatens to dismantle these lifelines, leaving vulnerable populations without access to critical health services. From January 2005 to May 2024, a staggering 219 rural hospitals in the United States closed or converted to facilities without inpatient services. Understanding and addressing the causes of these closures is a matter of urgent concern.
Collaborative Networks - A Path to Sustainable Rural Healthcare
Rural hospitals across the nation are facing mounting challenges—rising costs, limited resources, and increasing demands for quality care. In response, organizations like Rough Rider and Headwaters have come together to form clinically integrated networks (CIN) designed to strengthen rural healthcare systems through collaboration and shared resources. This model, which aligns with national trends, leverages collective expertise to expand care access, reduce administrative burdens, and align with evolving payer models.
The Growing Challenges of Medicare Advantage: Implications for Hospitals and Critical Access Facilities
As Medicare Advantage (MA) continues to grow in popularity, hospitals, particularly Critical Access Hospitals (CAHs), are finding themselves grappling with new challenges. While MA plans offer expanded benefits to beneficiaries, they present significant financial and operational obstacles to healthcare providers. From delayed and denied payments to increased administrative burdens, these challenges are threatening the financial stability of hospitals, especially those that serve rural communities.