Moving from Identification to Action - The Next Phase of Healthcare Process Improvement (LEAN form)
After identifying waste and inefficiencies in healthcare operations (December 13, 2024 blog), organizations must transition into the critical implementation phase of process improvement. This article examines the methodology and systematic approach required to transform improvement opportunities into measurable results.
Successful process improvement initiatives begin with a comprehensive analysis of current operations. This analysis must extend beyond surface-level observation to capture the actual state of processes, workflows, and operational patterns. Process documentation is the cornerstone of this analysis, encompassing standard operating procedures, workflow patterns, resource utilization, communication protocols, and system dependencies.
Establishing a performance baseline constitutes another critical element of current state analysis. Organizations must measure and document patient throughput metrics, resource utilization rates, quality indicators, staff productivity measures, and cost efficiency metrics. This comprehensive baseline provides the foundation for measuring future improvements and ensuring accountability throughout the implementation process.
Managing People, Process, and Plan - A Systematic Approach to Organizational Success
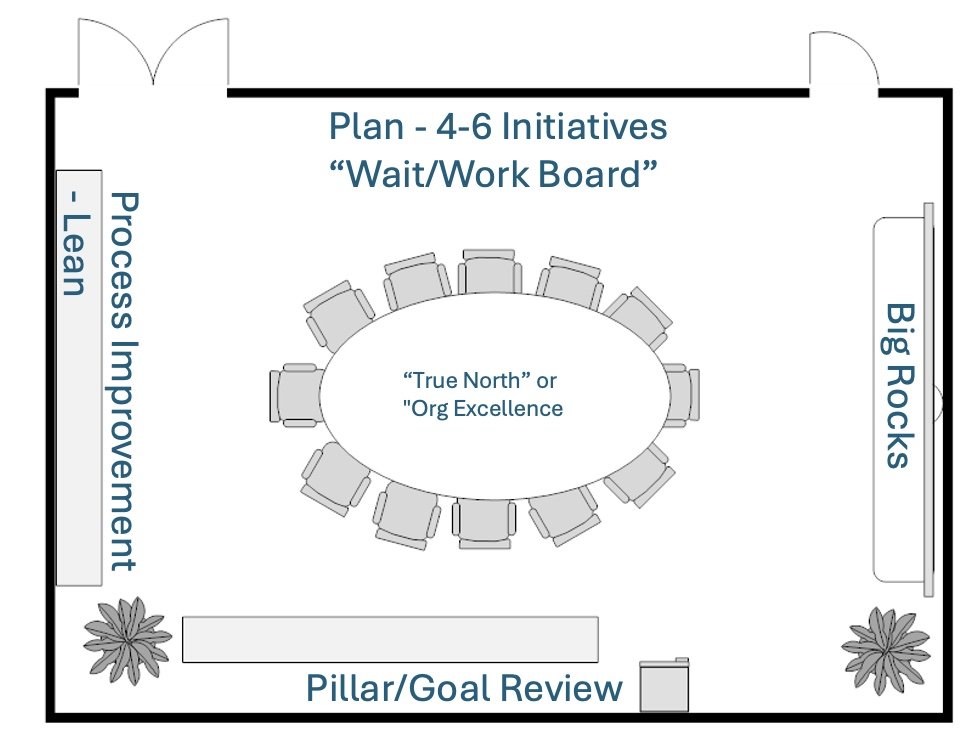
In many healthcare organizations, the key to achieving success lies in effectively managing People, Process, and Plan. To truly harness this triad, it requires a disciplined, structured approach that keeps the entire team aligned with the organization’s mission, strategic goals, and improvement initiatives. One highly effective method for maintaining this alignment and keeping progress on track is what I call the "Around-the-Room Review."
This blog will explore how to set up a structured review process by utilizing the physical layout of a room to track progress and address key strategic priorities in a systematic way.
Creating Synergy Between People and Process: Using Lean to Improve Emergency Department Efficiency and Patient Experience
Emergency departments (EDs) are a pivotal point of entry for patients requiring urgent medical attention, making ED efficiency a critical metric for hospitals. The Centers for Medicare & Medicaid Services (CMS) developed several performance measures to track how well hospitals manage patient flow, including the measure OP-18b: the median time from emergency department arrival to emergency department departure for discharged patients. This measure, while commonly used as a benchmark for time-based performance, is more than just a number. It reveals opportunities for improving patient flow, reducing bottlenecks, and enhancing overall patient experience through effective teamwork and process optimization.
By leveraging Lean Process Improvement principles, hospitals can reduce inefficiencies and enhance coordination between departments, allowing patients to move more seamlessly through the emergency department. But achieving these results requires more than just good processes—it requires a synergy between the people working at the front lines of patient care and the processes designed to streamline their work. This article explores how a thoughtful combination of “People” and “Process” can help hospitals not only meet the CMS OP-18b standard but also significantly improve the quality of care and the patient experience.
Book Review: “Patient-Centered Strategy” by Jeff Hunter
"Patient Centered Strategy" by Jeff Hunter provides a comprehensive guide for healthcare leaders looking to transform their organizations by focusing on patient-centered care. The book argues that by putting patients at the center of strategic decision-making, healthcare organizations can achieve better clinical outcomes, higher levels of patient satisfaction, and greater operational efficiency. It’s a strategic approach that balances patient needs with the overarching goals of healthcare providers, aligning the two for mutual benefit.
Hunter offers a roadmap for implementing this strategy, focusing on key areas such as leadership, organizational culture, operational excellence, and the adoption of value-based care models. He emphasizes that the transition to a patient-centered strategy is not just a superficial change in policy but a fundamental shift in how healthcare organizations operate.
The Power of Organizational Culture: How Strong Culture Elevates Staff Relationships and Patient Care
In healthcare, we often focus on clinical outcomes, patient satisfaction scores, and operational efficiency. But beneath these metrics lies something fundamental to every hospital’s success: its culture. A strong organizational culture isn’t just a buzzword—it’s the very foundation that supports positive staff relationships and enhances the quality of care patients receive.
When a hospital or healthcare organization fosters a healthy, supportive culture, the effects ripple through every aspect of the organization, from staff morale to patient outcomes. In contrast, when culture is neglected, even the best clinical practices can falter under the weight of disconnection and discontent.